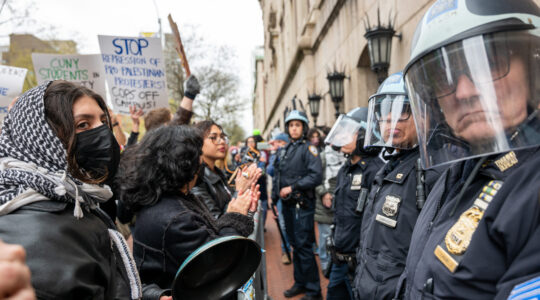Threading a needle on free speech, Jewish leaders demand Columbia rein in pro-Palestinian protests
Heads of outside organizations and the campus Hillel seek enforcement of university rules meant to safeguard Jewish and other students from harassment.